Cultural competence in United States medical education: a scoping review of implementation and evaluation practices
Neeti Swami, Haley Lewsey, Angelica Nibo, Radha Patel, Stephanie Stroever and Lauren Cobbs
Department of Medical Education, Texas Tech University Health Sciences Center School of Medicine, USA
Submitted: 19/03/2025; Accepted: 25/03/2026; Published: 09/04/2026
Int J Med Educ. 2026; 17:26-41; doi: 10.5116/ijme.69c3.e171
© 2026 Neeti Swami et al. This is an Open Access article distributed under the terms of the Creative Commons Attribution License which permits unrestricted use of work provided the original work is properly cited. http://creativecommons.org/licenses/by/3.0
Abstract
Objectives: The objective is to identify what is needed in Cultural Competence Curricula in medical schools and suggest a framework for evidence-based curricula that can be flexibly applied.
Methods: We conducted a scoping literature review of Cultural Competence Curricula in United States medical schools. After reviewing 160 articles, 77 met inclusion criteria for analysis. We collected qualitative data on curricula described in each article to analyze elements of curriculum structure, evaluation, and study design.
Results: Our results illustrate a high prevalence of structure styles conducive for quality learning, including longitudinality, integration, incorporation into clinical training, and experiential learning. The most common method for evaluating student learning was student self-evaluation with few programs performing reevaluations or utilizing patients as evaluators. Of knowledge, attitudes and skills, skills were least evaluated. Curricula with higher self-reported efficacy used a greater proportion of self-evaluations, while ones with lower self-reported efficacy used more external evaluations. Quasi-experimental study designs were more common in curricula with high self-reported efficacy.
Conclusions: Curriculum developers across the world can improve implementation of Cultural Competency Curricula by maximizing the quantity of structural components, having higher quality of evaluation, and connecting with the local community surrounding their medical school. To develop a robust curriculum, we encourage longitudinal multi-component learning in integrated courses evaluated via experimental and quasi-experimental study designs.
Introduction
Cultural Competence is a concept of relevance to medical schools all across the world as the impact of globalization continues to increase. Being a country with a diverse population, cultural competence has gained importance in the United States (U.S.) and its medical schools throughout time. Cultural competence is taught using many different structural formats across the U.S. that can be used in many different environments.
A Brief History of Cultural Competence
The notion of cultural competence was originally rooted in the social movements of the 1960s and 1970s. This tumultuous time brought attention to racial and cultural disparities through the civil rights movement, the gay rights movement, women’s liberation, environmentalism, and counterculture. The need to operate within a multicultural society led to the term cultural competence, coined in 1989 by Terry L. Cross.1 Following desegregation, the reality of unresolved injustices and health inequity in the United States was evidenced by the 2002 Institute of Medicine publication Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care which caused a shift in cultural group-specific knowledge to patient-centered frameworks.2 Subsequently, in 2003, the Liaison Committee on Medical Education (LCME) required medical students to demonstrate cultural competence upon graduation to ensure that future physicians are prepared to provide quality care to historically underserved groups, sparking nationwide reform in cross-cultural medical education by establishing a formal curricular standard.3,4
Cultural Competence Curriculum (CCC) is commonly defined in a medical context as education regarding knowledge, skills, and attitudes conducive for cross-cultural communication.5 This definition has provided a conceptual basis for the implementation of programs aimed at establishing cultural competence in their students. To acknowledge the diversity present throughout various populations, the definition of culture in education has expanded and includes race/ethnicity, gender, sexuality, religion, disability, and the historical and socioeconomic context that have led to health inequity for underserved groups.6-8
Since undergraduate medical education exists within varying political climates, the value and quality of cultural competence education is determined by the discretion of individual programs.4 For example, the approach to cultural diversity varies by program, and there is controversy around ‘political correctness’ and implementation of social justice curricula.9-11 Additionally, “competence” implies a stagnant point in knowledge acquisition, so many programs prefer the term “cultural humility” to embrace lifelong learning because culture is ever-changing.12-14
Observations in Current Literature
The literature reveals a vast array of definitions of culture and regional needs pertaining to the local communities surrounding the schools.6-8 This also means there is huge variability in the format of how CCC is taught. This increases challenges for standardization of development, implementation, and assessment of CCC, causing difficulty in identifying best practices and determining the impact of such practices on patient outcomes and health disparities.15 This also leads to many different educational structures. The literature currently has limited data that holistically shows and compares these curriculum structures while also connecting them with student outcomes and a best model for CCC implementation.
Medical CCC structure varies in terms of course length, frequency, rigor, level of integration, level of interaction, and experiential learning.16-18 However, there has been a historical evolution from the typical one-day didactic interventions of the 2000s and early 2010s toward instruction spread across up to four years.16,19-21 These longitudinal curricula also facilitate active learning by incorporating interactive learning activities due to increases in supporting evidence.16,19-21 Some cultural competence curricula remain isolated from basic science and clinical skills curricula while others have adopted an embedded approach.17,22 Modern curricula are increasingly emphasizing community partnership and cultural immersion with some regularly invite community members to speak on their experiences14 and others having students walk in the shoes of their fellow community members.18 Overall, these changes represent a trend toward curricular recognition of the complexity and intersectionality needed to guide student understanding of the sociocultural dynamics that impact patients.17,23,24
Success is often determined by formal or informal evaluation. Medical schools evaluate their CCC by utilizing either their students’ self-perceptions of their abilities, external evaluations assessed by another individual, team, third-party, and/or accreditation body.16,25,26 Several evaluation formats exist including surveys, focus groups, interviews, quizzes, tests, Objective Structured Clinical Exams (OSCE), thematic analyses, patient assessments, and community projects.16,25,26 While most articles include post-implementation performance or student-made reports of improvement, comprehensive evaluation methods and assessment of application of material in real-life scenarios is lacking.
In fact, current literature includes few instances of reevaluation or patient evaluation of students’ learning of cultural competence.27 Evaluations are instead often written and assessed by medical personnel such as faculty, medical students, and trained standardized patient actors, but not patients. Little to no programs utilize evaluations from patients due to challenges in asking patients to evaluate students which include obtaining Institutional Review Board (IRB) approval, risks for coercion, and limited time, resources, and patient interest. Hospital and clinical medicine runs off productivity which can discourage using extra time to acquire feedback from patients regarding learner performance, and delivering feedback upstream is often not a straightforward process for medical staff.28,29 Many patients opt out because they believe their feedback will not be used, rendering the process meaningless for making change.29 However, a few programs found promising alternatives by inviting people representing specific cultural backgrounds to act as patients and evaluate medical students.6,30,31 Without a means of evaluating retention of material over time or patient response to students who have participated in CCC, we may not be ensuring that future physicians will practice cultural competence that patients feel truly benefits them. Studies suggest medical students may overestimate their culturally sensitive skills compared to knowledge assessments and that all CCC has had little to no effect on patient satisfaction or outcomes.15,32 This indicates that despite curricular developments over the past few decades, current non-patient-centered assessments remain unsuccessful at pointing out the cross-cultural gaps that patients identify as needing improvement, perpetuating physician unpreparedness to respond to real-world needs.
Review Question and Objectives: Identifying Components of Effective CCC
Upon starting medical school, we embarked on our professional journeys with a desire to become physicians capable of creating a more equitable healthcare system.33,34 As a result, we took note of how cross-cultural instruction and social determinants of health were embedded into the medical school curriculum. We found that successful CCC are made up of many elements that each contain variability, and saw a gap in the literature where best practices for curriculum structure and evaluation need further identification.17,21,35,36 Thus, our review focuses specifically on structural components and their relationship to the efficacy of CCC.
We examined the manner in which educators design CCC for student benefit in the short-term and patient benefit in the long-term. Since the variability in training and evaluation methods makes it difficult to identify best practices and the effects on patient outcomes, this paper focuses on the following research question: What are the current needs and ways to improve the structural implementation of evidence-based CCC at United States medical schools? Related objectives include: (1) to elucidate the current state of CCC educational formats in U.S. medical schools, (2) to identify the current key structural components of CCC, given the attempted changes over time in CCC delivery, (3) to determine how to appraise the efficacy of key structure components and (4) to observe whether quality of assessment can be attributed to study design.
Existing scoping reviews of the structure of CCC describe evaluation methods and the prevalence of curricular components in narrative synthesis without cross-comparison between elements.27,37 A 2023 review from Li and colleagues synthesized cultural competence frameworks and models and created an actionable guide using an Acceptance Commitment and Training (ACT) cultural model.23 Our scoping review similarly investigates structural elements of CCC, but is innovative in its analysis of the relationship between those elements and student learning outcomes. We suggest a framework that promotes teaching models with positive reports of efficacy in implemented CCC for other curriculum developers to reference when creating their own CCC. Though our framework has specific recommendations for the structure of CCC, there are successful curricula that do not fall strictly within the guidelines in our review. In this review, efficacy is defined by the extent to which a program met their desired outcomes according to each included article. In addition, our review is comparative between papers and focused on efficacy in relation to unique elements such as curriculum structure and evaluation methods. It provides a robust qualitative analysis via descriptive statistics and offers suggestions for increasing patient evaluations. Thus, this paper focuses on curriculum structure, efficacy, and evaluation techniques of CCC; it does not delve into the content of the curricula at this time.
Methods
Search Strategy
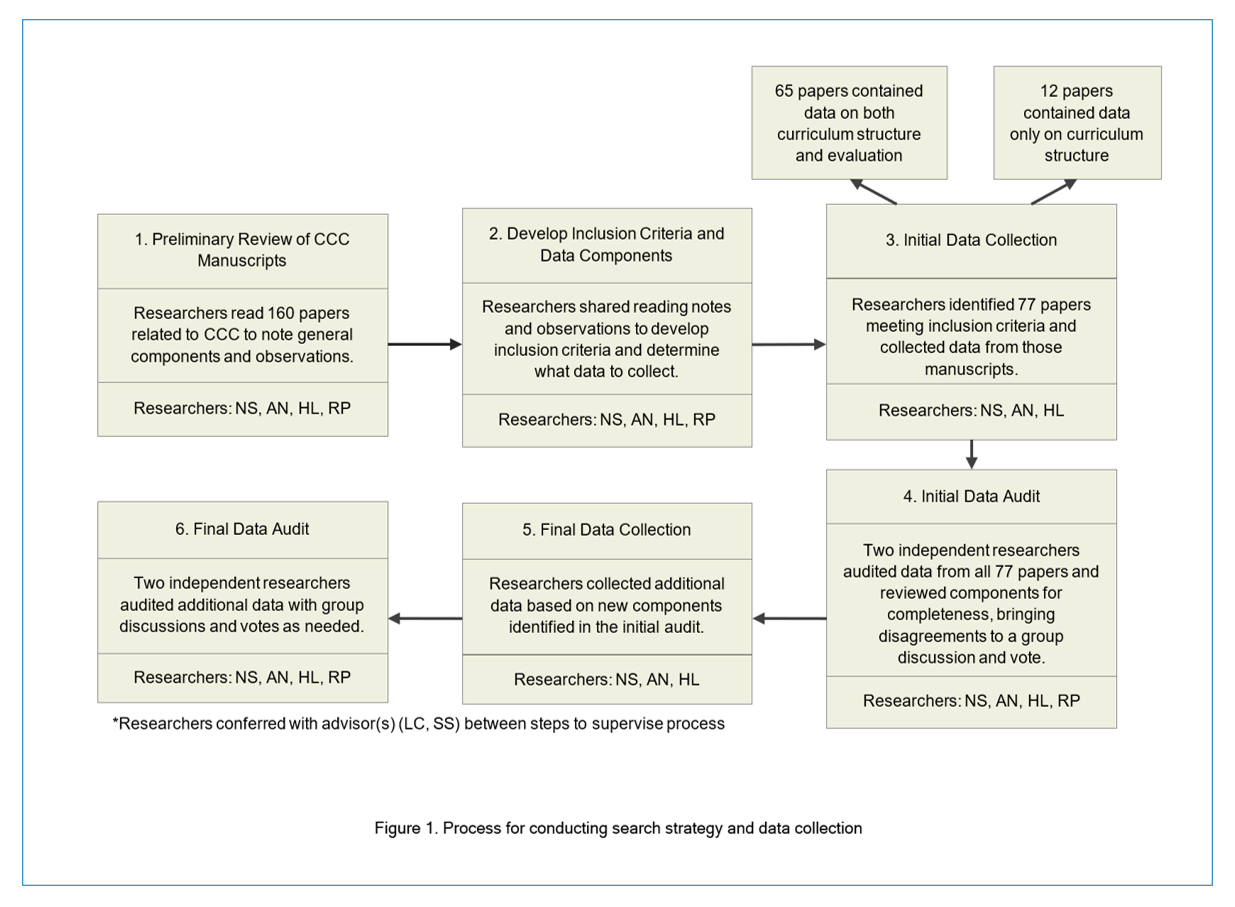
We performed an initial search of Google Scholar, Scopus, Ovid, and PubMed aimed at locating published studies on the topic, with the latest review in March 2023 (see Figure 1 for search strategy and data collection process). The text words contained in the titles and abstracts of relevant articles, and the index terms describing the articles were used as key terms in the search strategy. We developed key words by finding index articles and identifying their key words, then refining the search iteratively to land on the best search strategy that would yield the most comprehensive results. Consistent keywords including “cultural competence curriculum,” “medical school,” “education,” and “cultural competence” were used in all databases along with various boolean operators. Other keywords included, but weren’t limited to, "cultural humility curriculum," “multicultural curriculum,” "curriculum," "training," "program," and “cultural education.” We also used citation analysis to further enhance our sample and continued reviewing until saturation was met. We also had routine meetings as the search was run to maintain consistency. During preliminary review of CCC articles, publication year, regional differences, public funding, course structure, content preferences, definitions of cultural competence, variance in teaching methodology, and reported outcomes were noted. Due to no human participants being directly involved in the methodology of this study, risks were considered minimal and no IRB approval was needed.
Study Selection
After preliminary reading and discussion of 162 articles, we reached a consensus on elements and their operational definitions for qualitative data collection. Citations of these articles were collated and uploaded into EndNote 21 (Clarivate, London, UK) and duplicates removed. One-hundred sixty unique articles were identified in total. Inclusion criteria and data components were developed at this time. Per Joanna Briggs Institute (JBI) methodology, following initial data collection, articles were screened by two or more of our team members for assessment against the inclusion criteria for the review.38 Seventy-seven articles were included and eighty-three articles from the total 160 were excluded.
Inclusion and Exclusion Criteria
All articles analyzed in the scoping review had a description of a CCC enacted in an individual U.S. Doctor of Medicine (M.D.) medical school. Only U.S. M.D. schools were included since all of their cultural competence curricula operate under LCME requirements. The purpose of this study was to identify the best approaches to teaching cultural competence topics in undergraduate medical education. Thus, the articles needed to have commented on either curriculum structure and/or evaluation on the efficacy of their program to be included in the study. Only studies published in English were included because the United States M.D. schools publish their articles primarily in English. Additionally, there were limited resources for translating and reviewing articles in other languages. Studies published since 1989 were reviewed as this was when the term cultural competence was coined, with the earliest included study being published in 1994.1 Articles that covered programs taking place across multiple medical schools, were non-M.D., or took place outside of medical school were excluded. Programs that did not give information on their curriculum structure or program evaluation were also excluded.
This scoping review included articles with both experimental and quasi-experimental study designs consisting of randomized controlled trials, non-randomized controlled trials, before and after studies, and interrupted time-series studies. In addition, analytical observational studies such as prospective and retrospective cohort studies and case-control studies were included. This review also included descriptive observational study designs like case series. Qualitative studies focused on qualitative data including, but not limited to designs such as phenomenology, grounded theory, qualitative description, and action research were not excluded.
Seventy-seven articles covering CCC structure and/or evaluation of outcomes were identified. Of these 77 articles, 65 articles contained information on both curriculum structure and evaluation.
Data Extraction and Synthesis
For initial data collection, two or more of our team members independently extracted qualitative data from the articles included in the scoping review by using a review methodology based on the JBI scoping methodology.38 To maintain consistency between team members during data extraction and synthesis, all team members were trained to collect data based on agreed upon operational definitions based on each term in the context of CCC, expanded upon in Table 1. Using a qualitative approach to document these previously defined elements, final extracted curriculum data included details on structural components, attendance requirements, local community involvement, study design, methods of evaluation, evaluated constructs of cultural competence, and efficacy remarks. “Efficacy” in this review is defined by the extent to which programs achieved their desired outcomes. For the purpose of analysis, curriculum structure components included Integration, Longitudinality, Clinical Training, Experiential Learning, Interactive Activity, Passive Learning, Mandatory, and/or Optional. Study design elements included Pre-Curriculum Evaluation, Quasi-Experimental and Post-Curriculum Evaluation. Methods of evaluation included the elements of External Evaluation, Self-Evaluation, Reevaluation, and Patient Evaluation. The elements of evaluated cultural competence constructs included Knowledge, Skills, and Attitudes. These findings were tabulated on a master spreadsheet. All data underwent a final audit by at least two trained researchers. Any disagreements between independent reviewers were arbitrated by a third reviewer. The spreadsheet data was then reviewed with descriptive statistics and depicted graphically to summarize and compare the results.
Results
The presentation of results includes a descriptive summary of data collected on curriculum structure and program evaluation, followed by summaries of the cross-comparisons performed between elements. For the purpose of this review, “structural components” refer to different aspects of a curriculum’s design, not limited to teaching methods and course duration. For analysis, “efficacy” was defined by the curriculum’s low, medium, or high level of achievement of the article authors’ desired outcomes.
Descriptive Summary of Curriculum Structure
Data on curriculum structure was divided into nine elements: Mandatory and Optional attendance, involvement of a Local Community near the school, and a focus on Integration, Longitudinality, Clinical Training, Experiential Learning, Interactive Activity, and Passive Learning (see Table 1). Throughout this paper, these elements are referred to as “structural components.” Analysis of curriculum structure demonstrated Passive Learning to be most commonly utilized, with presence in 97% (n=77) of curricula. Longitudinality, Clinical Training, and Integration with other existing courses were the least commonly utilized, each found in less than 55% (n=77) of curricula. All schools used at least two of the six main components, and 19% (n=77) of schools used all six. The most common quantity of structure components incorporated was four components, present in 31% (n=77) of curricula.
Descriptive Summary of Curriculum Evaluation
Analysis of curriculum evaluation was divided into three categories: Method of Evaluation, Constructs Evaluated, and Efficacy.
Data on competence assessment was gathered by observation of the cultural competence constructs that programs evaluated. The category ‘Constructs Evaluated’ was further divided into evaluation of Knowledge, Skills, and Attitudes. Of these constructs, Attitudes were the most evaluated at 94% (n=77), while Skills were the least evaluated at 72%.
Method of Evaluation was divided into Study Design and four assessments of student learning: External Assessment, Self-evaluation, Reevaluation, and Patient Evaluation. Self-evaluation was found to be the most common assessment method, employed in 83% (n=65) of curricula, while External Evaluation was used in 68% of curricula. Reevaluation and Patient Evaluation were utilized the least, at 15% (n=65) and 6.2%, respectively.
Regarding study design, the majority of programs utilized either a Post-Curriculum Evaluation only or a Quasi-Experimental (pre and post) design, with 52% (n=65) and 45% usage respectively. Very few programs used a Pre-Curriculum Evaluation only or a Randomized Controlled Trial study design, at less than 1.5% (n=65) usage each.
Cross-Comparison: Structure and Efficacy Findings
Cross-comparison of curriculum structure to efficacy revealed the most commonly implemented combinations of structure components in relation to the level of efficacy.
Each of the 25 observed curriculum structure combinations were labeled A through Y from most to least frequently implemented. Of the five most frequent structure combinations, combination A (n=15: Integration, Longitudinality, Clinical Training, Experiential Learning, Interactive Activity, and Passive Learning) and combination E (n=5: Integration, Clinical Training, Interactive Activity, and Passive Learning) had the most evaluations with high efficacy (A with 80% and E with 100%). Meanwhile, combination B (n=10: Interactive Activity and Passive Learning) and combination C (n=9: Experiential Learning, Interactive Activity, and Passive Learning) had the most evaluations with low efficacy (B with 10% and C with 11%). Programs using five or six structural components did not have low efficacy reports.
Of the schools with documented Efficacy, 35% (n=65) had involvement with local cultural groups. The programs with a local aspect of content had a higher percentage of high efficacy evaluations than those without this aspect, at 87% (n=23) compared to 76% (n=42). Additionally, local-focusing programs had fewer low efficacy evaluations, at 4.4% (n=23) compared to 14% (n=42).
Cross-Comparison: Evaluation and Efficacy Findings
The curricula evaluated themselves through only Self-evaluation, only External Evaluation, or through a combination of both Self-evaluation and External Evaluation. After cross-comparing curriculum evaluation and efficacy, analysis demonstrated High Efficacy Curricula to have the highest proportion of solely Self-Evaluations, at 35% (n=52). Medium Efficacy Curricula used a combination of Self and External Evaluation most often, at 67% (n=6), while using only Self-Evaluation the least, at 17%.
As for study design, only 1 High Efficacy curriculum (1.9%, n=52) used a Randomized Controlled Trial, and only 1 Low Efficacy curriculum (14%, n=7) used a Cross-Sectional Pre-Curriculum study. Post-Curriculum Evaluations were most common for Low and Medium Efficacy curricula, at 71% (n=7) and 67% (n=6), respectively. Quasi-Experimental study designs were most common for High Efficacy programs at 50% (n=52).
Discussion
Countries around the world are comprised of countless communities, each with their own culture. Especially with increased globalization and diversification of communities, teaching medical providers how to understand and acknowledge the impact of their shared lived experiences is necessary for optimizing health outcomes. This review offers a robust analysis of the successes and limitations of Cultural Competence Curricula (CCC) in order to depict its current state and identify quality implementation frameworks for future use. These observations for strengths, weaknesses, and best practice can be applied to CCC curriculum around the world. Though most programs we observed incorporate passive learning and promote student self-reflection, our results suggest that many may have missed opportunities to implement more engaging learning formats, ensure long-term retention, and gather external input from affected populations.
Structure: What’s Needed?
Over 30% of programs did not incorporate Integration, Longitudinality, and presence in Clinical Training into their CCC, suggesting that there is a widespread lack of these elements in CCC. The paucity of these structural components indicates that many programs lack opportunities for students to reinforce learning through repetition and usage in clinical rotations. Though not considered in this review, longitudinal CCC extending into graduate medical education is an additional opportunity for reinforcement.39,40 Furthermore, without integration and engagement with this content during clinical training, students may not be connecting cultural competence to their growing scientific and clinical knowledge or to real patients. CCC can implement discussion-based settings, cross-cultural content in science blocks, and activities in the clinical years to help students increase cognitive processing, repetition, and application of material.41
Evaluation: What’s Needed?
Our findings suggest that programs do not consistently assess all three domains of cultural competence: knowledge, skills, and attitudes. Skills are assessed the least, which demonstrates that some programs may not be assessing or emphasizing the importance of cross-cultural communication strategies. This could also be due to difficulty acquiring enough diverse standardized patients and resources like interpreters for relevant OSCEs. Schools may have difficulty hiring people willing to work sporadically as independent contractors or difficulty budgeting for the high costs of their services.42,43 However, skills are not to be prioritized over knowledge and attitudes. Students should leave medical school with increased knowledge of cultural norms and self-awareness, having potentially challenged their long-standing views.44 Additionally, developing a wider knowledge base, such as a greater understanding of historical factors, will prepare students to face health disparities visible during their clinical encounters.44 Discordance between knowledge, skills, and attitudes could lead to reduced student preparedness and hinder patient-physician interactions.
Our results reveal that many programs heavily relied on self-evaluations by students which suggests that success is being measured by perceptions of students and/or faculty rather than affected patients. Though this allows students to be introspective, it could lead to faculty and students perceiving their competence as higher than the reality. The interpersonal nature of cultural competence may affect the validity of intrapersonal evaluations like self-evaluations.45 As demonstrated in our findings, the curricula that intentionally discuss challenges and were deemed low or medium efficacy utilized external evaluations more heavily. This may indicate that without outside input from affected populations or bodies of cultural knowledge, some areas for improvement may be missed. We encourage all programs to consider using external rather than self-evaluation methods in order to be self-critical.45 As mentioned by multiple papers, self-evaluations are subjective: while they reflect student perspective, it does not indicate measurable growth or excellence in applied skills. However, for programs who would like to use self-evaluation to encourage self-reflection, we also recommend adding external evaluations to gain valuable and measurable information alongside student insight.46-48
The purpose of these aforementioned measures is to improve patient outcomes. Our review depicts a lack of patient evaluations, which represents a need for more patient input as patient satisfaction is the ultimate determinant of efficacy. Though patient evaluation is lacking, it is challenging to correct without an established model that addresses the previously mentioned barriers to organizing a standardized patient pool representative of populations in CCC.29,42,43 However, some programs have successfully overcome this challenge. For example, a 2013 study by Thew et al. provides a successful example of patient recruitment as they recruited and compensated deaf volunteers from the local community to participate in role-play exercises with medical students.49 Using community volunteers reduces costs and risk of coercion, allows for schedules that are appropriate for the volunteers’ and learners’ time, and enables true representation of the target patient population(s) in the curriculum. Four of our included studies describe patient evaluation models that CCC developers believe created more comprehensive learning experiences and were all deemed successful overall.6,31,50,51 We encourage programs to reflect on the few existing examples of patient evaluation and create a model that is both generalizable and manageable for patients and educators.
Cross-comparisons: Recommendations for Best Practice
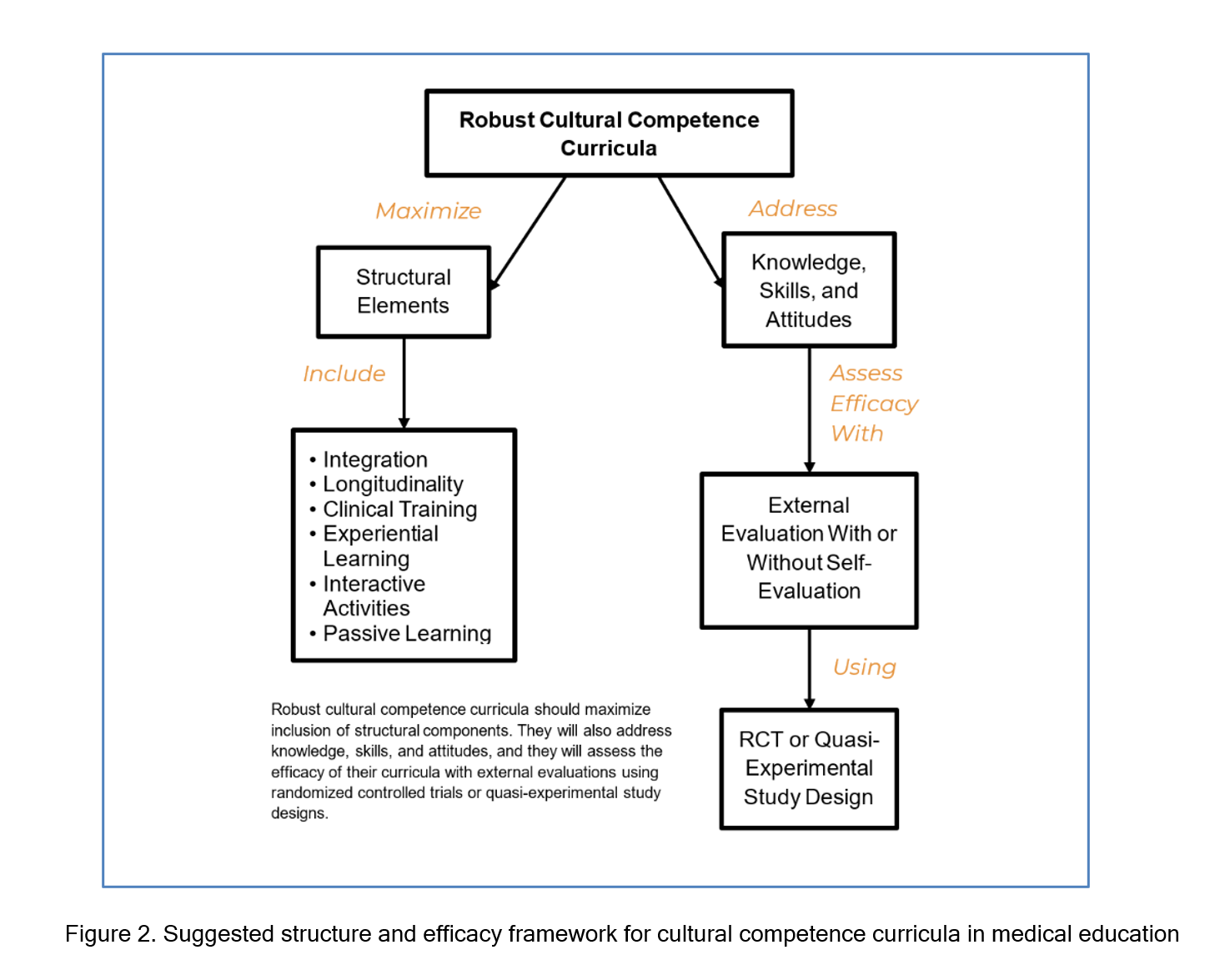
Based on our findings, we have a suggested framework for curriculum structure and evaluation. Many of these findings are corroborated by other frameworks which share overlapping features such as the importance of community engagement, reviewing knowledge, skills, and attitudes, and different forms of student engagement.17,23,52,53 This framework, depicted in Figure 2, consists of maximal structure components, external evaluations jointly assessing knowledge, skills, and attitudes, and strong study design. It appears that successful programs maximize the quantity of structural elements, connect with the local community, and have higher quality evaluations.
Though our results suggest that several iterations of structure combinations can be effective, it seems that the quantity of components is a major factor. By incorporating more structural components, students will experience more varied reinforcement of cultural competence to provide them with more opportunities to engage with the material.54 Additionally, involvement of a community surrounding the school allows students to connect with real people, hear their stories, and see the real impact of cultural competence on them.55 Finally, we encourage programs to use higher quality study designs to build the strength of the literature for others to reference. Using pre- and post-evaluations or randomized controlled trials allows programs to establish a baseline, modify the curriculum according to the learning gaps specific to their students, and limit unaccounted variables affecting the success of a curriculum.
We acknowledge that there are other factors besides structure and efficacy that affect CCC improvement including faculty buy-in, student motivation or lack thereof, lack of diverse workforce, limited budget for interpreters, and access to cultural competence staff training.56,57 However, regarding structure and efficacy, this framework provides a more meaningful educational experience to students and may be significant for the continued betterment of cultural competence education in medicine.
Global Importance and Relevance
Developing a medical school curriculum that teaches cross-cultural communication is important internationally. Every country has various communities with different lived experiences that can benefit from CCC. Certain populations are universally found around the world, such as those who are women, low socioeconomic status, disabled, rural, LGBTQ+, etc., who benefit from culturally competent care.58-60 Some elements of cultural competence such as social determinants of health, cross-cultural communication, and bias similarly affect patients worldwide.61-63
Moreover, like those in this review, programs across many countries often have specific populations with cultural considerations that impact health, such as migrant populations in Europe,60 aboriginal populations in Australia,64 and language barriers in South Africa.65 Based on the findings from our review, we recommend that curriculum developers involve these communities in their CCC so that students learn practical applications of cultural competence to their unique environment. Regardless of nation, teaching CCC is associated with better patient outcomes and can improve patient interactions,66,67 and many recognize the need to implement and improve CCC.67,68 Our paper provides curriculum structure recommendations on maximizing different learning methods, increasing the quality of student assessment, and encouraging better standards of study design that are applicable to designing and evaluating CCC anywhere in the world.
Strengths and Limitations of This Review
As a scoping review, the authors acknowledge this work may not exhaustively include all scholarship on this topic. We do believe it is nonetheless a robust representation of the available literature in this area. Strengths of this review include the comprehensive methodology and depth of analysis specific to curriculum structure and program evaluation of the implementation of these curricula. Not only did we descriptively detail the usage of key structural components, but we connected and stratified usage by reported efficacy to highlight potential predictors of success for curriculum developers.
One of our main limitations was the qualitative, subjective nature of the articles, which prompted us to develop our own definitions of many elements. Some of these definitions, such as Low, Medium, and High Efficacy, were based on claims made by each article without objective standardization between articles for what constituted an efficacious curriculum. Observations were limited by what was explicitly stated, so it is possible that our data did not accurately represent a curriculum if its published paper lacked documentation of any aspect.
Conclusions
Overall, curriculum development is extremely multifaceted. Our review suggests that the best practices include developing a longitudinal interactive curriculum that is integrated with clinical and basic sciences. It would also be beneficial for programs to work towards incorporating reevaluations and most importantly, patient evaluations. In the future, we plan to compose additional reviews that examine the content of the CCC articles and thematically analyze important aspects of cultural competence curricula that we have yet to discuss. In addition, we plan on introducing a patient assessment model to the Texas Tech University Health Sciences Center School of Medicine where patients from target cultural groups evaluate our students’ cultural competence. Future reviews can form other cross-comparisons, use our elements with newer publications, perform objective analyses of curriculum effectiveness, or examine the structural makeup and evaluation of CCC in more countries. As we continue improving upon cross-cultural education, we must remain steadfast in striving to empower patients to give us feedback and in looking for progress in quality of care.
Acknowledgements
We would like to acknowledge and thank Texas Tech University Health Sciences Library for their support of our literature search.
Conflict of Interest
The authors declare that there is no conflict of interest.
References
- Cross TL, Dennis KW, Isaacs MR. Towards a culturally competent system of care: a monograph on effective services for minority children who are severely emotionally disturbed. 1st ed. Washington, DC: Georgetown University Child Development Center; 1989.
- Institute of Medicine (US) Committee on Understanding and Eliminating Racial and Ethnic Disparities in Health Care. Unequal treatment: confronting racial and ethnic disparities in health care. Smedley BD, Stith AY, Nelson AR, editors. Washington (DC): National Academies Press (US); 2003.
- Crosson JC, Deng W, Brazeau C, Boyd L and Soto-Greene M. Evaluating the effect of cultural competency training on medical student attitudes. Fam Med. 2004; 36: 199-203.
PubMed - Cultural competence education for medical students. Association of American Medical Colleges; 2005. [Cited 16 Oct 2025]; Available from: https://www.aamc.org/media/20856/download.
- Shapiro J, Lie D, Gutierrez D and Zhuang G. "That never would have occurred to me": a qualitative study of medical students' views of a cultural competence curriculum. BMC Med Educ. 2006; 6: 31.
Full Text PubMed - Woodard LJ, Havercamp SM, Zwygart KK and Perkins EA. An innovative clerkship module focused on patients with disabilities. Acad Med. 2012; 87: 537-542.
Full Text PubMed - Betancourt JR and Cervantes MC. Cross-cultural medical education in the United States: key principles and experiences. Kaohsiung J Med Sci. 2009; 25: 471-478.
Full Text PubMed - Wong JW and Omori J. Medical School Hotline: cultural competency in serving the homeless in Hawai'i at the John A. Burns School of Medicine. Hawaii J Med Public Health. 2016; 75: 18-21.
PubMed - Diaz J. Florida Gov. Ron DeSantis signs a bill banning DEI initiatives in public colleges. National Public Radio; 2023 [cited 16 Oct 2025]; Available from: https://www.npr.org/2023/05/15/1176210007/florida-ron-desantis-dei-ban-diversity.
- Wong A. DEI came to colleges with a bang. Now, these red states are on a mission to snuff it out.: USA Today; 2023 [cited 16 Oct 2025]; Available from: https://www.usatoday.com/story/news/education/2023/03/23/dei-diversity-in-colleges-targeted-by-conservative-red-states/11515522002/.
- Yang M. Greg Abbott signs law banning diversity offices in Texas higher education. Guardian Media Group; 2023 [cited 16 Oct 2025]; Available from: https://www.theguardian.com/us-news/2023/jun/14/new-texas-bans-law-diversity-offices-state-higher-education.
- Alpert A, Kamen C, Schabath MB, Hamel L, Seay J and Quinn GP. What exactly are we measuring? Evaluating sexual and gender minority cultural humility training for oncology care clinicians. J Clin Oncol. 2020; 38: 2605-2609.
Full Text PubMed - Lekas HM, Pahl K and Fuller Lewis C. Rethinking cultural competence: shifting to cultural humility. Health Serv Insights. 2020; 13: 1178632920970580.
Full Text PubMed - Juarez JA, Marvel K, Brezinski KL, Glazner C, Towbin MM and Lawton S. Bridging the gap: a curriculum to teach residents cultural humility. Fam Med. 2006; 38: 97-9102.
PubMed - Vella E, White VM and Livingston P. Does cultural competence training for health professionals impact culturally and linguistically diverse patient outcomes? A systematic review of the literature. Nurse Educ Today. 2022; 118: 105500.
Full Text PubMed - Crandall SJ, George G, Marion GS and Davis S. Applying theory to the design of cultural competency training for medical students: a case study. Acad Med. 2003; 78: 588-594.
Full Text PubMed - Dao DK, Goss AL, Hoekzema AS, Kelly LA, Logan AA, Mehta SD, Sandesara UN, Munyikwa MR and DeLisser HM. Integrating theory, content, and method to foster critical consciousness in medical students: a comprehensive model for cultural competence training. Acad Med. 2017; 92: 335-344.
Full Text PubMed - Godkin M and Weinreb L. A pathway on serving multicultural and underserved populations. Acad Med. 2001; 76: 513-514.
Full Text PubMed - Thom DH, Tirado MD, Woon TL and McBride MR. Development and evaluation of a cultural competency training curriculum. BMC Med Educ. 2006; 6: 38.
Full Text PubMed - Lubimir KT and Wen AB. Towards cultural competency in end-of-life communication training. Hawaii Med J. 2011; 70: 239-241.
PubMed - Vasquez Guzman CE, Sussman AL, Kano M, Getrich CM and Williams RL. A comparative case study analysis of cultural competence training at 15 US medical schools. Acad Med. 2021; 96: 894-899.
Full Text PubMed - Kumagai AK and Lypson ML. Beyond cultural competence: critical consciousness, social justice, and multicultural education. Acad Med. 2009; 84: 782-787.
Full Text PubMed - Li S, Miles K, George RE, Ertubey C, Pype P and Liu J. A critical review of cultural competence frameworks and models in medical and health professional education: A meta-ethnographic synthesis: BEME Guide No. 79. Med Teach. 2023; 45: 1085-1107.
Full Text PubMed - Powell Sears K. Improving cultural competence education: the utility of an intersectional framework. Med Educ. 2012; 46: 545-551.
Full Text PubMed - Miller E and Green AR. Student reflections on learning cross-cultural skills through a 'cultural competence' OSCE. Med Teach. 2007; 29: 76-84.
Full Text PubMed - Burson RC, Familusi OO and Clapp JT. Imagining the 'structural' in medical education and practice in the United States: A curricular investigation. Soc Sci Med. 2022; 300: 114453.
Full Text PubMed - Brottman MR, Char DM, Hattori RA, Heeb R and Taff SD. Toward cultural competency in health care: a scoping review of the diversity and inclusion education literature. Acad Med. 2020; 95: 803-813.
Full Text PubMed - Flanagan OL and Cummings KM. Standardized patients in medical education: a review of the literature. Cureus. 2023; 15: 42027.
Full Text PubMed - Sheard L, Peacock R, Marsh C and Lawton R. What's the problem with patient experience feedback? A macro and micro understanding, based on findings from a three-site UK qualitative study. Health Expect. 2019; 22: 46-53.
Full Text PubMed - Litzelman DK and Cottingham AH. The new formal competency-based curriculum and informal curriculum at Indiana University School of Medicine: overview and five-year analysis. Acad Med. 2007; 82: 410-421.
Full Text PubMed - Symons AB, McGuigan D and Akl EA. A curriculum to teach medical students to care for people with disabilities: development and initial implementation. BMC Med Educ. 2009; 9: 78.
Full Text PubMed - Seeleman C, Suurmond J and Stronks K. Cultural competence: a conceptual framework for teaching and learning. Med Educ. 2009; 43: 229-237.
Full Text PubMed - Novak DA, Hallowell R, Llobrera K, Schreiber J, Wright E and Elliott D. Stances toward anti-racist medical education: a qualitative analysis of critical consciousness in first-year medical students. AERA Open. 2022; 8: 23328584221103878.
Full Text - Ward J and Randall V. From college graduate to physician: professional identity formation. MedEdPublish (2016). 2020; 9: 180.
Full Text PubMed - Seeleman C, Hermans J, Lamkaddem M, Suurmond J, Stronks K and Essink-Bot ML. A students' survey of cultural competence as a basis for identifying gaps in the medical curriculum. BMC Med Educ. 2014; 14: 216.
Full Text PubMed - Berger JT and Miller DR. Health disparities, systemic racism, and failures of cultural competence. . Am J Bioeth. 2021; 21: 4-10.
Full Text PubMed - Deliz JR, Fears FF, Jones KE, Tobat J, Char D and Ross WR. Cultural competency interventions during medical school: a scoping review and narrative synthesis. J Gen Intern Med. 2020; 35: 568-577.
Full Text PubMed - Peters MD, Godfrey CM, McInerney P, Soares CB, Khalil H, Parker D. The Joanna Briggs Institute reviewers' manual 2015: methodology for JBI scoping reviews. Adelaide: The Joanna Briggs Institute; 2015.
- Fune J, Chinchilla JP, Hoppe A, Mbanugo C, Zuellig R, Abboud AT, Oboh O and Monica van de Ridder JM. Lost in translation: an OSCE-based workshop for helping learners navigate a limited English proficiency patient encounter. MedEdPORTAL. 2021; 17: 11118.
Full Text PubMed - Atkinson RB, Khubchandani JA, Chun MBJ, Reidy E, Ortega G, Bain PA, Demko C, Barreiro-Rosado J, Kent TS and Smink DS. Cultural competency curricula in US graduate medical education: a scoping review. J Grad Med Educ. 2022; 14: 37-52.
Full Text PubMed - Dolmans DH and Schmidt HG. What do we know about cognitive and motivational effects of small group tutorials in problem-based learning? Adv Health Sci Educ Theory Pract. 2006; 11: 321-336.
Full Text PubMed - Murphy S, Imam B and MacIntyre DL. Standardized patients versus volunteer patients for physical therapy students' interviewing practice: a pilot study. Physiother Can. 2015; 67: 378-384.
Full Text PubMed - Standardized patients frequently asked questions. UC Davis Health; 2025 [cited 16 Oct 2025]; Available from: https://health.ucdavis.edu/simulation/standardized-patients-faqs.html.
- Taylor R. Addressing barriers to cultural competence. J Nurses Staff Dev. 2005; 21: 135-142.
Full Text PubMed - Lin CJ, Lee CK and Huang MC. Cultural competence of healthcare providers: a systematic review of assessment instruments. J Nurs Res. 2017; 25: 174-186.
Full Text PubMed - Borowsky H, Morinis L and Garg M. Disability and ableism in medicine: a curriculum for medical students. MedEdPORTAL. 2021; 17: 11073.
Full Text PubMed - Hearn SL and Hearn PJ. Working with people with disabilities: an interactive video/lecture session for first- and second-year medical students. MedEdPORTAL. 2020; 16: 10913.
Full Text PubMed - Smothers ZPW, Tu JY, Grochowski C, Koenig HG. Efficacy of an educational intervention on students' attitudes regarding spirituality in healthcare: a cohort study in the USA. BMJ Open. 2019; 9(4): e026358.
- Thew D, Smith SR, Chang C and Starr M. The deaf strong hospital program: a model of diversity and inclusion training for first-year medical students. Acad Med. 2012; 87: 1496-1500.
Full Text PubMed - Green AR, Miller E, Krupat E, White A, Taylor WC, Hirsh DA, Wilson RP and Betancourt JR. Designing and implementing a cultural competence OSCE: lessons learned from interviews with medical students. Ethn Dis. 2007; 17: 344-350.
PubMed - Perlman A and Stagnaro-Green A. Developing a complementary, alternative, and integrative medicine course: one medical school's experience. J Altern Complement Med. 2010; 16: 601-605.
Full Text PubMed - Lombardero A, Assemi KS, Jacobs NN, Houmanfar RA, Trejo S and Szarko AJ. An acceptance and commitment training (ACT) framework for teaching cultural humility: a guide for translating act from a therapeutic context into a medical education curriculum. J Clin Psychol Med Settings. 2023; 30: 261-273.
Full Text PubMed - Hayes SC, Luoma JB, Bond FW, Masuda A and Lillis J. Acceptance and commitment therapy: model, processes and outcomes. Behav Res Ther. 2006; 44: 1-25.
Full Text PubMed - Giorgdze M, Dgebuadze M. Interactive teaching methods: challenges and perspectives. International E-Journal of Advances in Education. 2017; 3(9): 544-548.
- Sandy M, Holland B. Different worlds and common ground: community partner perspectives on campus-community partnerships. Michigan Journal of Community Service Learning. 2006; 13: 30-43.
- Solotke M, Sitkin NA, Schwartz ML and Encandela JA. Twelve tips for incorporating and teaching sexual and gender minority health in medical school curricula. Med Teach. 2019; 41: 141-146.
Full Text PubMed - Worden MK and Ait-Daoud Tiouririne N. Cultural competence and curricular design: learning the hard way. Perspect Med Educ. 2018; 7: 8-11.
Full Text PubMed - Colon-Gonzalez MC, El Rayess F, Guevara S and Anandarajah G. Successes, challenges and needs regarding rural health medical education in continental Central America: a literature review and narrative synthesis. Rural Remote Health. 2015; 15: 3361.
Full Text - Sorensen J, Norredam M, Suurmond J, Carter-Pokras O, Garcia-Ramirez M and Krasnik A. Need for ensuring cultural competence in medical programmes of European universities. BMC Med Educ. 2019; 19: 21.
Full Text PubMed - Sorensen J, Norredam M, Dogra N, Essink-Bot ML, Suurmond J and Krasnik A. Enhancing cultural competence in medical education. Int J Med Educ. 2017; 8: 28-30.
Full Text PubMed - Pineda P, Klenner M, Espinoza G, Mariño R and Zaror C. Intercultural sensitivity in Chilean healthcare profession students. BMC Med Educ. 2024; 24: 467.
Full Text PubMed - Lu PY, Tsai JC and Tseng SY. Clinical teachers' perspectives on cultural competence in medical education. Med Educ. 2014; 48: 204-214.
Full Text PubMed - Ogunlana MO, Oyewole OO, Aderonmu JA, Onyeso OK, Faloye AY and Govender P. Patterns and predictors of cultural competence practice among Nigerian hospital-based healthcare professionals. BMC Med Educ. 2023; 23: 933.
Full Text PubMed - Arnold-Ujvari M, Rix E, O'Donnell K and Kelly J. Cultural education provided to renal staff caring for first nations people in australia and similarly colonized countries: a scoping review. J Ren Care. 2025; 51: 70023.
Full Text PubMed - Grant T. Problems of communicative competence in multi-cultural medical encounters in South African health services. Curationis. 2006; 29(4): 54-60.
- Ho MJ, Yao G, Lee KL, Beach MC and Green AR. Cross-cultural medical education: can patient-centered cultural competency training be effective in non-Western countries? Med Teach. 2008; 30: 719-721.
Full Text PubMed - Lanting K, Dogra N, Hendrickx K, Nathan Y, Sim J and Suurmond J. Culturally competent in medical education - European medical teachers' self-reported preparedness and training needs to teach cultural competence topics and to teach a diverse class. MedEdPublish (2016). 2019; 8: 98.
Full Text PubMed - Rahman U and Cooling N. Inter-cultural communication skills training in medical schools: a systematic review. Medical Research Archives.. 2023; 11: .
Full Text - Haidet P, Morgan RO, O'Malley K, Moran BJ and Richards BF. A controlled trial of active versus passive learning strategies in a large group setting. Adv Health Sci Educ Theory Pract. 2004; 9: 15-27.
Full Text PubMed